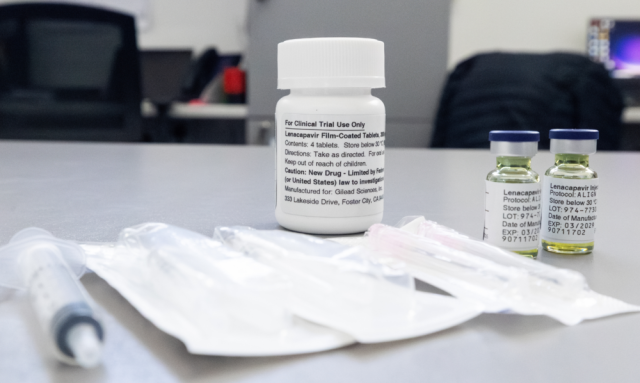
Amid the mostly depressing HIV headlines of recent times, concerned as they mainly are with the deadly impacts of donor defunding, South Africa’s imminent roll-out of a twice-yearly HIV prevention injection called lenacapavir (LEN) has been a spot of bright light.
Staff in 360 healthcare facilities spread across the country stand trained and ready to receive and administer the drug, which has been found to be near perfectly successful in preventing HIV when administered twice yearly, attracting cliches like “game-changer”, “groundbreaking” and “new dawn”, although contrarian voices warn that the public benefit of rapid LEN roll-outs in African contexts is far from clear.
Now is not the time to drop the ball, to use another cliché, but many in the HIV space take comfort in the knowledge that the person responsible is Hasina Subedar, the health department’s senior technical adviser in HIV prevention.
Getting Subedar to give an interview took some convincing (she eschews the limelight) but she ultimately took a call on a Saturday afternoon in late April, with LEN all but ready to launch.
After some connectivity issues — “Is this better? Hang on, I’ll move closer to the modem. Hello, Hello, He-LO-HO … ” — Subedar tries to minimise the achievement.
“It’s not my first, um … ”
“Rodeo?” I interject, with too much enthusiasm.
“Roll-out!”
Before LEN, Subedar oversaw the roll-out of a once-a-day HIV prevention pill (a form of pre-exposure prophylaxis or PrEP medication) for HIV-negative South Africans wanting to protect themselves against infection, becoming, former health department director-general Yogan Pillay told me, “one of the most experienced people in understanding PrEP provision and one of its leading advocates”.
When I exclaim about the responsibility she shoulders, Subedar chuckles and says: “I don’t get stressed easily. I am on a high all the time. I just have to keep moving and things have to run like clockwork.”
She works from 6am to 11pm every day and typically takes off only from 16 December, the Day of Reconciliation, until 3 January. Last year, however, she worked through.
“I had to sit and finish all the training materials [for clinic staff to be able to administer LEN], while worrying over consignments of drugs that still needed to come into the country,” says Subedar, who for the past nine months has met weekly with all the organisations involved in supplying the drug, a process she describes as “immensely complex and at times quite fraught”.
“Relax your grip and there’s a chance the drugs will simply not make it into the country. I have had to become a very hard taskmaster for people who don’t do the things they’re supposed to be doing,” she says.
Grit, grace and humour
With the drugs now in the country, the next step is getting LEN to those most likely to benefit from it, a challenge made markedly trickier by the Trump administration’s funding cuts to South Africa, which, according to a report released by Physicians for Human Rights and partners in April, have undermined much of the infrastructure — such as community-based testing and field recruitment for HIV prevention services — needed to create demand for LEN.
How will such yawning gaps be bridged?
In answering, Subedar focuses on the opportunity inherent in decreased donor funding.
“Previously, with the oral PrEP roll-out, we had donors telling us: ‘This is where you must implement. These are the populations you must implement for.’ It was initially led by them [donors] and this often resulted in fragmented service delivery.

“With LEN, I was determined that it would be government-led and not rolled out by partner-funded projects but instead integrated within public primary healthcare from the outset.”
If questions remain about the viability of the plan (a prominent HIV researcher told me that Subedar “is constantly having to make things work in a sea of mediocrity”), her competency is widely acknowledged.
Francois Venter, the executive director of Ezintsha at the University of the Witwatersrand, recognised Subedar’s work ethic and “absolute integrity”. Desmond Tutu Foundation chief executive Professor Linda-Gail Bekker praised her ability to work well with a spectrum of roleplayers, “doing so with grit, grace and humour”.
These are not innate abilities. How, I wonder aloud, were they forged?
“I’m from Pietermaritzburg,” Subedar begins, as if this on its own answers the question.
“I was born there, in Edendale Hospital. My father was a tailor who wanted a boy but instead my mother had five girls, so I was often dressed like a boy from the time I was little,” she says.
Subedar’s parents, Hajira and Goolam Subedar, were both largely self-taught people, denied education by family circumstances.
“It was important to them that we should receive the education they were denied. My father always said: ‘The one thing you must always do is educate yourself because nobody can ever take away your education,’ which is so true.”
The Subedar family lived towards the bottom end of East Street (renamed Masukwana Street in 2014), near the mosque. For junior school, the girls attended the Nizamia School, 200m from their home but had to walk much further for senior school, to Pietermaritzburg Indian Girls’ High School, on Berg Street.
Subedar says she was “non-conformist” and found the compulsory afternoon sport “quite challenging”. “You had to find a way of ducking out if somehow or other,” she says.
As the middle child, she was often left to fend for herself, never quite included in the alliances of her two elder and two younger sisters. This would prove consequential.

The Subedars were a political family who often shared what little they had with the families of Robben Island detainees like Harry Gwala. Subedar’s father decided that one of his daughters should go and live in the home of another detainee, Abdool Kader Hassim, to support his wife Nina and two young sons.
“My older sisters flat out refused and since my younger sisters were too young, it pointed at me,” says Subedar, admitting that she resented the imposition initially but came to appreciate the experience.
“Our own home was a tiny little place, with the bathroom and toilet separate outside. For hot water you had to make a fire below a copper geyser but when I went to live with Nina and her boys I had my own room and I learnt a lot.
“I became more politicised around this time, which wasn’t unique to me. It was a common experience in the areas and communities we lived in but it shaped my thinking. There wasn’t this thing of we are Indian and they are African. We were very integrated in lots of ways.”
The other force shaping Subedar’s outlook was money, or rather the lack of it.

“My father’s work completely dried up when I was at high school, so I had to work to support myself,” says Subedar, who dropped out of a social work degree after just one year due to a lack of funds.
Her choice to study nursing was born mainly out of need — she would be able to study and earn, enabling her to support the family — but there was something else.
“When I was 18 years old I was attacked by a man who tried to kill me. I was left badly injured: two of my fingers were completely severed and a third was left non-functional,” she recalls.
Amid the chaos of the emergency, the nurses who attended to Subedar in hospital provided a refuge of calmness and kindness.
“My hair had lots of glass and sand in it and one of the nurses said: ‘Let me wash your hair for you.’ And that meant so much to me,” she says, confirming that the experiences of care strongly factored in her decision to study nursing.
Subedar says she emerged from the experience a more compassionate person, “especially towards those experiencing rupture in their lives” and resolved to move forward “without any self-pity — without ever talking about it, in fact — while finding ways to compensate for the considerable loss of functionality in my left hand”.
The black section and the white section
Within a month of applying to train as a nurse, Subedar was on her way to Cape Town, to learn and work in Groote Schuur Hospital, where “there was a black section and a white section and you stayed on your side!” (Ever the non-conformist, Subedar found ways of undermining workplace apartheid, playing squash late at night “at the white residence where we were not allowed to be”).
In Pietermaritzburg, Subedar had been well aware of the inequality in the education system. Now, she saw it up close in the health system.
“One of the things I did as a student was go into Langa to train people in first aid. Ambulances weren’t going into Langa at night and in many instances people died at the police station for want of basic care.”
Subedar qualified as a professional nurse and spent some time working in intensive care units, until her son was born, at which point she returned to Pietermaritzburg to be closer to her family, taking a position as a mental healthcare nurse at Fort Napier, the psychiatric hospital and later as part of an outreach team in Durban communities like Chatsworth, Phoenix and Merebank.
“It was a refreshing change, more humane in many respects, because I could spend time with people who were dealing with life in all of its complexity,” she says.
When she was granted long leave in 1989, Subedar used it to further her studies at the University of KwaZulu-Natal, where she was ultimately offered a post providing clinical training to student nurses in both psychiatry and midwifery.
Having left Cape Town with a diploma in nursing, Subedar managed, by 1993, to complete a basic degree, a qualification in nursing education, an honours in psychology and a master’s in mental health nursing, all while working and raising a son as a single parent.
“Shame, I moved around and this poor child moved everywhere with me. At one point he said to me: ‘Mom, you are very lucky you have me as a son,’ and that is so true because he never complained, he just adjusted every time.”
After South Africa’s first democratic elections in 1994, Subedar, who had participated in some of the strategic teams that had been set up in advance to look at the transformation of healthcare, decided to move back to the Western Cape, feeling that of all the provinces, its mental health services were the most in need of transformation, concentrated as they were in psychiatric hospitals like Valkenberg, Lentegeur, Stikland and Alexandra.
“One of the reasons I left academia to go back into the [public health] system was to contribute to the realisation of the idea that basic services should be taken out of hospitals and made available in communities,” says Subedar, who spent three hopeful years — from 1997 to 2000 — working on the establishment of community mental health services in the Western Cape, only to become frustrated with the province’s see-saw politics.
“We had three health MECs in that period with different political affiliations and I think this influenced the direction in which we went, which was not what I had envisaged,” she says.
In 2000, Subedar was headhunted to work at the South African Nursing Council as its registrar, opening a new and distinct chapter in her life.
“I was the first female registrar and the first person of colour to hold that position,” says Subedar, recalling that the discourse on transformation when she entered the council, “was at the level of worrying about what new pictures to put on the walls and which building names should change, not about the profession and what needed to happen to transform it”.
“We had this changing health system, which is also needing to respond to new challenges like the HIV/Aids pandemic. For me, one of the priorities was making sure that our professionals are able to work in such a system,” says Subedar, who instigated a review of the scope of practice of nurses, with appropriate adjustment to their education.
The South Africa’s Nursing Act of 2005 was largely based on the new frameworks Subedar developed and she believes it “clearly defines what nurses should be doing and what the regulations are and making sure that those regulations enable the nurses to do what they have to do.”
The next step was to have been the transformation of the nursing education system. “That’s the part that …” she starts to say, but her voice peters out. She doesn’t need to describe the crisis in nursing education in South Africa currently, which has been well publicised.
Instead of necessary transformation, nursing education has been compressed by the closure of several nursing colleges and choked by changing qualification requirements, contributing to a situation in which nearly half of all nurses registered with the South African Nursing Council are over the age of 50.
Subedar’s time at the council ended badly. In 2008, controversially, her contract was not renewed, leading her to take legal action. She was reinstated for a short time but departed in 2009.
“I didn’t know what to do at that point but an opportunity arose to come back into the department to assist with the healthcare re-engineering process. It was this question of ‘how do we restructure primary healthcare and make it more functional in the current system?’”
Learning from scratch
So began her time “of sort of developing stuff for the department and delivering for them”.
When she was asked to roll out HPV vaccination in 2012, it was a one line instruction: “You will roll out the HPV vaccination, it will be in March 2013 and a treasury allocation will be made available but only in April 2013,” Subedar recalls, mirthfully.
“There was no pilot, yet we had to reach every public school within 20 days, campaign style. I learnt a few valuable lessons in all that. You need to know how many people are required for the work and to understand who is going to do what.
“Your people need to be competent and they need to be supported. Do they understand their role? Do they have job aids [tools such as checklists, algorithms and explanatory posters]? Those campaigns were scripted to the T,” she says, adding, “the beauty of all of this is that people, once they have direction and know what they need to do, they get it done, especially at the province level.”
Typically, whenever she has taken on a new project for the department, Subedar has started in complete unfamiliarity.
“On the day I was approached about HPV vaccination, I did not know what it was. I did not know how it needed to be administered. I knew nothing but this was a strength because I needed to systematically grasp the subject.
“I learnt from scratch on PrEP, too,” says Subedar, who advocates, “seeking out the experts and literature on the clinical trials and studies and getting them to provide you with all the technical information that is required for the direction that you need to go and then just shaping it, so that it will work in the real world in which you want to implement”.
The consultative approach has not been without its challenges.

“With oral PrEP, I sat in the very first meeting with these incredibly forceful HIV researchers and everybody was doing their own study and had their own ideas about what should be done and which population we should be focusing on, be it men who have sex with men, adolescent girls, sex workers or transgender people.
“Disappointment was guaranteed,” says Subedar, insisting her personal motto remains “collaboration”.
“I might not agree with you but I will listen. All stakeholders should have a space to give their view, including civil society. It [collaboration] doesn’t come naturally to the department of health but if anybody tries to create animosity or start excluding people, I would intervene,” she says, before politely ending the conversation.
A difficult problem has arisen and for once it has nothing to do with her work.
“I am renovating and the contractor failed to cover my room, so everything — my clothes, my linen, my floors — is coated in a fine layer of dust.”
This story was produced by the Bhekisisa Centre for Health Journalism. Sign up for the newsletter.
Amid the mostly depressing HIV headlines of recent times, concerned as they mainly are with the deadly impacts of donor defunding, South Africa’s imminent roll-out of a twice-yearly HIV prevention injection called lenacapavir (LEN) has been a spot of bright light. Staff in 360 healthcare facilities spread across the country stand trained and ready to




